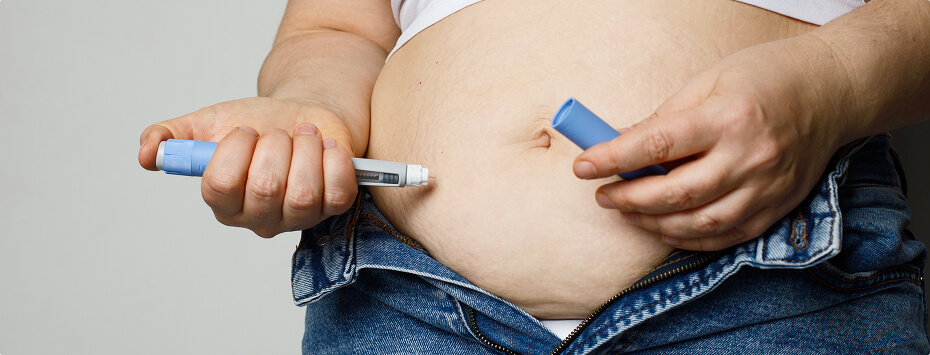
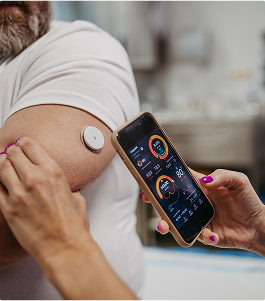
Pre-bariatric surgery optimisation refers to the medical, nutritional and lifestyle steps taken before surgery to optimise the patient for a safe procedure and successful long-term weight management. It focuses on correcting metabolic imbalances, improving overall fitness and reducing risks linked to obesity-related conditions.
- Improving metabolic health — strengthening cardiovascular, liver and hormonal function to support safer surgery.
- Stabilising hormone and glucose levels — managing insulin resistance, thyroid issues if present and diabetes for better intra-operative control.
- Reducing surgical risks — lowering complications related to anaesthesia, bleeding, infection and wound healing.
- Enhancing recovery and long-term outcomes — Improving post-operative healing and ensuring sustained weight-loss.
Why optimisation prior to bariatric surgery matters
Optimisation before bariatric surgery is essential for ensuring a safer procedure and creating the right physiological conditions for effective, long-lasting weight loss. It helps reduce medical complications, improves organ function and supports a smoother recovery.
- Lower anaesthetic and surgical risks — better cardiovascular and respiratory stability reduces complications during the operation.
- Better blood sugar and blood pressure control — stabilising these levels minimises peri-operative risks and supports wound healing.
- Reduced risk of blood clots and postoperative complications — optimising mobility, circulation and metabolic health decreases thrombosis (blood clot) risk.
- Improved liver size and quality for safer surgery — pre-operative diets and medication like GLP-1 help reduce the size of an enlarged, fatty liver, allowing easier surgical access.
- Stronger nutritional and psychological readiness — ensures patients are prepared for the lifelong dietary and behavioural changes required after surgery.
Medical evaluation before bariatric surgery
A thorough medical evaluation helps identify any health issues that need attention before surgery. These assessments guide personalised optimisation plans, reduce peri-operative risks and ensure that the procedure is carried out as safely as possible.
- Full metabolic and endocrine review — assessing diabetes, thyroid disorders, lipid abnormalities and hormone balance.
- Comprehensive blood tests — checking glucose, HbA1c, liver function, kidney markers, iron levels, vitamins and B12 status.
- Sleep apnoea assessment — screening for obstructive sleep apnoea, which affects anaesthesia safety and postoperative recovery.
- Cardiovascular risk screening — evaluating heart health, blood pressure and potential cardiac concerns before surgery.
- Medication review and adjustments — ensuring current medications are safe and appropriately managed before the operation.
Lifestyle and nutritional optimisation before bariatric surgery
Lifestyle and dietary adjustments play a crucial role in preparing the body for bariatric surgery. These changes help reduce liver size, improve metabolic stability and build the habits needed for long-term weight-loss success.
- Pre-operative weight reduction strategies — gradual weight loss lowers surgical risks and enhances operative visibility.
- Dietitian-guided meal planning — structured nutrition plans ensure adequate protein, balanced macronutrients and improved metabolic control.
- High-protein, low-carbohydrate pre-surgery diet — supports fat loss, reduces liver size and stabilises blood glucose.
- Reducing sugary drinks, alcohol and smoking — minimises inflammation, improves healing and supports safer anaesthesia.
- Physical activity planning — introducing sustainable exercise routines to improve fitness, stamina and postoperative recovery.
Endocrine and metabolic management before bariatric surgery
Many people preparing for bariatric surgery have underlying hormonal or metabolic conditions that may or may not be related to obesity that need to be optimised for safety. Managing these issues early helps stabilise glucose control, support hormonal balance and reduce the risk of complications during and after the procedure.
- Obesity-related insulin resistance — improving insulin sensitivity to stabilise blood glucose and reduce peri-operative risks through weight loss or medication.
- Type 2 diabetes optimisation — adjusting medications and improving control to prevent complications during fasting and recovery.
- Thyroid disorder management — ensuring thyroid hormone levels are stable for optimal metabolism and surgical safety.
- PCOS management — addressing hormonal imbalances that may affect weight, glucose levels and postoperative outcomes.
- Correction of vitamin D, iron and B12 deficiencies — replenishing low nutrient levels to support healing and prevent postoperative fatigue or anaemia.
Weight-loss medications before bariatric surgery
In most cases, medications may be recommended to help reduce weight, stabilise metabolic health and lower surgical risks before the procedure. These treatments can be especially helpful for patients with severe obesity or uncontrolled diabetes.
- GLP-1 agonists — medications that improve satiety, support weight loss and enhance glucose control before surgery.
- Metformin — a safe option for improving insulin sensitivity and stabilising blood sugar levels.
- Other doctor-guided pharmacological aids — additional medications used when appropriate to support weight reduction and metabolic optimisation.
- Expected benefits and precautions — helping patients understand likely outcomes, potential side effects and medical monitoring requirements.
Preparing the liver for safer bariatric surgery
Many patients with obesity have an enlarged or fatty liver, which can make bariatric surgery technically difficult. A structured liver-shrinkage programme helps reduce liver size, improving surgical visibility and lowering the risk of complications.
- Importance of reducing liver size — a smaller, healthier liver allows better access to the stomach during surgery.
- Very low-calorie diets (VLCDs) — short-term, medically supervised diets designed to reduce liver fat efficiently.
- Duration and expected outcomes — typically followed for 1–4 weeks, depending on individual needs and surgical recommendations.
What to expect in the weeks leading up to bariatric surgery
The final preparation phase ensures your body is stable, your nutritional status is adequate and all medical conditions are well controlled. These steps help create the safest environment for your operation and recovery.
- Follow-up schedule — regular appointments to monitor weight, glucose levels and blood pressure before surgery.
- Repeat assessments — updated blood tests and clinical checks to confirm readiness for anaesthesia and operative safety.
- Final dietary instructions — guidance on VLCDs, hydration and pre-operative fasting based on your surgeon’s protocol.
- Medication adjustments — review of diabetes, blood pressure or anticoagulant medications to ensure safe dosing.
- Pre-admission preparation — instructions on what to bring, when to arrive and how to prepare on the day of surgery.
Potential risks if bariatric surgery optimisation is not ensured
Skipping or incompletely following pre-operative optimisation can increase the likelihood of complications and affect long-term weight-loss outcomes. Proper preparation ensures that the body is medically stable and ready for the demands of bariatric surgery.
- Higher surgical complications — increased risk of bleeding, infection and longer operative times when metabolic issues are unmanaged.
- Poorer wound healing — micronutrient deficiencies or uncontrolled diabetes can slow recovery.
- Unstable metabolic status — irregular glucose levels, thyroid imbalance or untreated sleep apnoea can complicate anaesthesia and recovery.
- Longer recovery with reduced weight-loss success — lack of preparation may lead to poorer post-operative adaptation and slower progress.
Summary
Pre-bariatric surgery optimisation is a crucial part of preparing for a safe and successful weight-loss procedure. By addressing medical, metabolic, nutritional and psychological factors ahead of time, patients enter surgery with greater stability and lower risk.
This groundwork not only improves surgical safety but also strengthens long-term outcomes by establishing healthier habits, correcting deficiencies and supporting hormonal and glucose balance. With structured guidance and personalised care, patients are better equipped for smooth recovery and sustained weight-loss success after bariatric surgery.
If you are planning bariatric surgery or want to understand how to prepare effectively, schedule a consultation with The Metabolic Clinic for a comprehensive pre-surgery optimisation programme tailored to your health needs.
Frequently Asked Questions (FAQs)
Optimisation reduces surgical and anaesthetic risks by stabilising metabolic health, improving nutrition and preparing the body for the demands of bariatric surgery.
Most patients require several weeks to a few months, depending on their metabolic status, weight, nutritional needs and specialist recommendations.
You may undergo blood tests, hormonal assessments, sleep apnoea screening and cardiovascular checks to ensure your body is safe for surgery.
Many patients benefit from losing a modest amount of weight beforehand, which helps reduce liver size, lower surgical risks and improve postoperative recovery. It is also indicative of long-term weight control if weight can be reduced pre-operation.
It is a short-term, low-calorie diet designed to reduce fat in the liver, making bariatric surgery safer and technically easier.
Yes, if deficiencies in vitamin D, iron, B12 or other nutrients are identified, supplementation helps correct them before the procedure.
Diabetes does not prevent surgery, but blood sugar must be optimised beforehand to reduce complications and support safer recovery.
Certain medications, such as blood thinners or some diabetes drugs, may be adjusted. Your doctor will guide you through safe modifications.
Yes, both increase the risk of complications. Patients are encouraged to stop smoking and reduce alcohol intake well before surgery.
Light to moderate physical activity improves fitness, enhances lung and heart function, and supports smoother recovery.
Correcting deficiencies is essential. Poor nutrition can slow healing and increase postoperative risks.
Yes, medications like GLP-1 agonists may be used to reduce weight and stabilise blood sugar in selected patients. It is now often considered the optimal standard of care prior to bariatric surgery where feasible.
Our care team will confirm readiness once your medical tests, nutritional status and lifestyle adjustments meet pre-surgery requirements.